By David Tuller, DrPH
There is a lot going on in the ME and ME/CFS world that I don’t get around to. That’s why I’m always grateful that Jennie Spotila always deconstructs the numbers on the annual spending claims from the National Institutes of Health. Last month, on her blog Occupy M.E., Spotila submitted the NIH’s 2020 numbers to her usual sharp analysis. I am reposting it in full here with her permission.
**********
The 2020 NIH Funding Fact Check
By Jennie Spotila
It is time, once again, for my annual NIH funding fact check. And, once again, NIH’s numbers do not add up. NIH claims to have spent $15 million on ME/CFS research in 2020. In reality, NIH spent slightly under $13 million.
Every year, NIH publishes its internal calculation of how much it spent on research in over 200 categories. These numbers are generally accepted as accurate and authoritative by Congress and the public alike. Over the years, however, I have found that the reported amount for ME/CFS does not stand up to closer examination as can be seen in this graph.
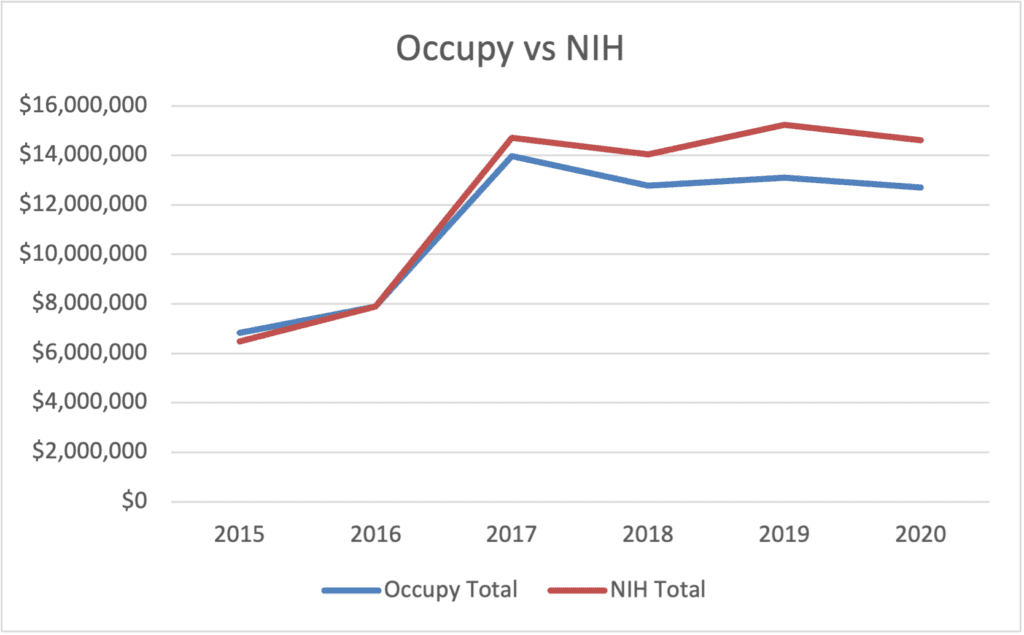

The trend continued in 2020. NIH claims that it spent $14.6 million in 2020, but this includes an extra $1.9 million that was not spent on ME/CFS research. The problem, as it has been for several years, is the amount NIH counts in intramural spending.
Intramural funding stays within NIH for research. There are almost 6,000 scientists at NIH and approximately 10% of NIH’s total budget supports their work. NIH’s intramural research related to ME/CFS was quite small for many years. Before 2017, intramural spending on ME/CFS was far less than 10% of the total spending.
However, in 2017 Dr. Avindra Nath’s ME/CFS Clinical Study began bringing subjects to NIH for extensive inpatient testing. Some of that testing was provided by other labs, such as the Human Energy and Body Weight Regulation Core and a lab studying Pathophysiology of Involuntary Movements and Volitional Disorders. NIH started counting the funding for these entire projects as ME/CFS spending, even though only a very small portion of the lab’s work was on ME/CFS.
The source of the problem seems to be NIH’s internal accounting process, as I explained last year. Intramural labs do not always receive funding earmarked to individual diseases or projects. The labs are also not required to track and report the way resources were allocated across projects. When NIH compiles the data for its Categorical Spending Chart, the full amount of funding to a lab is included in multiple categories even if the money was actually divided among multiple diseases.
As a result of this lack of rigor and specificity, NIH has included large amounts of funding in its ME/CFS number that were never spent on ME/CFS research. In 2019, the unrelated spending was close to $2 million for a study of involuntary movement disorders. Similar unrelated spending was included in 2018 and 2017. Last year, Dr. Vicky Whittemore assured me she was working with the staff who code studies for Reporter to try and fix this overestimate.
No unrelated intramural labs or studies were included in NIH’s calculation for 2020, so superficially it appears the problem was fixed. However, Reporter loaded on extra money in a different and less transparent way by using indirect costs.
In 2018 and 2019, Dr. Nath’s study received $750,000. But in 2020, NIH reports that Dr. Nath received an eye-popping $2.6 million–more than three times what he received in 2019. This huge jump in funding was especially surprising because pandemic restrictions interrupted Dr. Nath’s ability to bring study participants on site for extensive testing.
I asked Dr. Nath how the extra $1.9 million in funding was used, and he told me that he only received $750,000. Next I contacted Dr. Vicky Whittemore, and she told me that the excess $1.9 million added to Dr. Nath’s grant represented indirect costs for use of the Clinical Center facilities. The funding page for Nath’s study does not break the funding down into direct and indirect costs, as pages for many other studies do. This creates the appearance that Dr. Nath received far more money for the ME/CFS study than he actually did.
Perhaps it is a coincidence, but the excess amount on Dr. Nath’s grant is very similar to the excess amounts associated with the unrelated studies in 2017 through 2019, as I have previously reported. When I inquired, neither Dr. Nath nor Dr. Whittemore could tell me if the full $1.9 million of indirect costs were related to the ME/CFS study or to Dr. Nath’s many other studies. Furthermore, these indirect costs have never been charged to the ME/CFS study in previous years, and it’s unclear why the staff at Reporter changed the allocation in 2020.
The big problem is that adding those indirect costs to Nath’s ME/CFS study artificially inflates NIH’s ME/CFS funding number by almost $2 million. Once again, the picture of ME/CFS funding at NIH looks much better than reality.

Can’t only go after bad statistics re PACE. Plenty here.
“The source of the problem seems to be NIH’s internal accounting process,”
No, the problem is called “CORRUPTION” and NIH has plenty. People still seem to think that a PR program is real research. Public Relations programs only line pockets.
I still don’t understand why no one ever echoes this sentiment (other than sheer exhaustion) but in no particular order, here is the angry word-salad these reports create in my mind: FOIA REQUESTS. DISABILITY & DISCRIMINATION CLASS ACTION LAW SUIT. ACLU. CONGRESSIONAL HEARINGS ON WHETHER FRAUD, CORRUPTION OR NEGLIGENCE LEFT 15MILLION AMERICANS VULNERABLE TO LONG COVID ME/CFS.
The potential to win a suit is immaterial. The exposure of this issue and who has been behind it when combined with reality of long Covid really becoming apparent has more potential to help us than ANY advocacy or well written journal article. We all need to stop discussing amongst ourselves how much we all agree that we are passengers on the good ship Insanity. We already concur. Can we please play offense now?
simple accounting is even an issue when it comes to ME/CFS