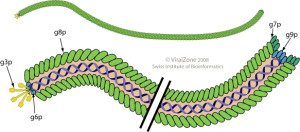

Pseudomonas aeruginosa is an important human pathogen which is a particular problem in patients with cystic fibrosis. The ability of this bacterium to form biofilms in the lung is linked to its ability to cause chronic infections. Pseudomonas aeruginosa biofilms contain large numbers of filamentous Pf bacteriophages (pictured). These viruses lyse cells and release DNA, which becomes one component of the biofilm matrix.
Mixing supernatants of P. aeruginosa cultures with hyaluronan, which is present in airways of cystic fibrosis patients, resulted in the formation of a biofilm – in the absence of bacteria. A major component of P. aeruginosa biofilms was found to be Pf bacteriophages. When purifed Pf bacteriophages were mixed with hyaluronan, biofilms formed. Similar biofilms also formed when the filamentous bacteriophage fd of E. coli was mixed with hyaluronan. Mixtures of Pf bacteriophages and various polymers (alginate, DNA, hyaluronan, polyethylene glycol) formed liquid crystals (matter in a state between a liquid and a solid crystal).
Pf phages were detected in sputum from patients with cystic fibrosis, but not in uninfected patients. Addition of Pf phage to sputum from patients infected with P. aeruginosa made the samples more birefringent, a property of liquid crystals. Compared with a strain of P. aeruginosa that does not produce Pf phage, colonies of virus-producing strains formed liquid crystals. These observations indicate that Pf phage help organize the bacteria into a biofilm matrix.
Some features of biofilms include their ability to adhere to surfaces, to protect bacteria from dessication, and to increase resistance to antibiotics. Addition of phage Pf increased biofilm adhesion and tolerance against dessication. Such addition also made the biofilm more resistant to aminoglycoside antibiotics, because these were sequestered in the biofilm. No phage-mediated increased resistance to ciprofloxacin was observed, probably because this antimicrobial does not interact with polyanions of the biofilm as do aminoglycosides.
These results show that presence of bacteriophage in a biofilm of P. aeruginosa helps organize the matrix while contributing to some of its fundamental properties. It seems likely that filamentous phages of other bacteria will play roles in biofilm formation, suggesting that targeting the phages in these matrices could be effectie strategies for treating biofilm infections.

This is such an interesting article. I wonder if phage detection can be used as a sort of marker for biofilm formation in clinical respiratory specimens. That would be very useful in considering treatment options.
Pingback: Viruses help form biofilms | Viral Bioinformatics Resource Center
Pingback: Viruses help form biofilms | Plant, Microbe, Ph...
Pingback: Viruses help form biofilms | Kenzibit's Blog on Host Cell and Pathogen Interactions
Pingback: Viruses help form biofilms | mikrobiologija | ...
Pingback: Viruses help form biofilms | Exocytosis | Scoo...
Pingback: Viruses help form biofilms | Viruses and parasi...
Pingback: Viruses help form biofilms | Tools and tips for...