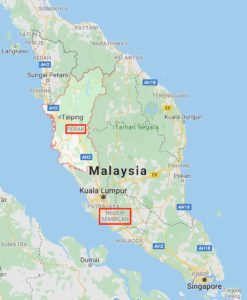

An outbreak of respiratory disease and encephalitis in pigs during 1998 took place in Ipoh City of Perak state in Malaysia (illustrated), and was followed by lethal encephalitis in patients associated with pig farming. Initially the pig disease was thought to be caused by classical swine fever virus, while the human disease was considered a result of infection with Japanese encephalitis virus (JE). Measures were taken to reduce mosquito populations by spraying, and immunizing workers with a JE vaccine. Neither measure slowed the epidemic.
By the end of 1998 the outbreak spread to Sikimat in Negeri Sembilan. The next year the disease spread to abattoir workers in Singapore. The movement of the disease was a consequence of transport of pigs from farm to farm in Malaysia, and to a slaughterhouse in Singapore (we now understand that most infected pigs do not show signs of disease). The outbreak in Malaysia ended when 1.1 million pigs were culled, and disease in Singapore stopped when importation of pigs from Malaysia was halted. A total of 283 human cases with 109 fatalities (39% fatality) was recorded.
A key player in the discovery of the cause of this outbreak was Kaw Bing Chua, who at the time was working at the University of Malaya. Chua had been working as a medical doctor until his 40s when he became frustrated with the profession. He was given a laboratory position at the University of Malaya and was there when the pig epidemic broke. His superiors thought the causative agent was JE virus but Chua thought otherwise. However because he had little virological experience he was ignored. Chua inoculated cell cultures with cerebrospinal fluid from one patient and observed the formation of syncytia, which would not be expected of JE virus. He brought the virus to the CDC at Ft. Collins, CO, which had responsibility for arboviruses. Work done there showed that the virus was not JE, and an electron micrograph suggested the presence of a paramyxovirus. Consequently the project was shifted to CDC in Atlanta, GA for further study.
Several years earlier (1994) an outbreak of respiratory and neurological disease in Australian horses and their trainers was ascribed to a Hendra virus, a newly discovered paramyxovirus. Given the similar disease in Malaysia and Singapore, experiments were done to determine if antibodies to Hendra Virus reacted with Chua€™s virus. The results showed that the Malaysian outbreak was due to a new Hendra-like virus, subsequently named Nipah Virus after the town of Kampung Sungei Nipah. There lived the patient whose CSF yielded the first virus isolate.
It was subsequently determined that Nipah virus had spilled over into pigs from its natural reservoir, fruit bats of the Pteropid species. Deforestation for pulpwood and industrial plantations in the previous 20 years had reduced the habitat of these bats. The severe haze that was a consequence of burning forests further reduced the ability of flying foxes to forage in fruit trees. Meanwhile, farmers had established piggeries in fruit tree orchards. Flying foxes attracted to these trees either contaminated pigs directly with virus-laden urine and feces, or dropped partly eaten and contaminated fruit on the ground which was then eaten by pigs. The pigs became infected and then passed on the virus to humans.
After this first Nipah virus outbreak, no subsequent infections of pigs in Malaysia or Singapore were reported, likely due in part to measures taken to improve biosecurity on pig farms to reduce the introduction of virus by flying foxes. However outbreaks of lethal Nipah Virus disease subsequently took place in Bangladesh and India. In the former country, infections were associated with consumption of contaminated date palm sap into which virus had been introduced via bat excreta. Infections in India are not associated with consumption of date palm sap, and the risk factors remain to be identified.
While Nipah virus infections continue to occur in India and Bangladesh, there are relatively few cases. Nevertheless, given the wide geographic distribution of fruit bats harboring the virus, and the absence of licensed vaccines and therapeutics, Nipah virus has been identified by WHO as one of 8 viruses with the potential to cause a public health emergency. As revealed at the Nipah Virus International Conference in Singapore, remarkable progress has been made on the development of vaccines and therapeutics. Nevertheless, a great deal of work remains to be done to establish rapid diagnostic tests, and to understand the factors that drive spillover of the virus from bats to humans and other animal species.
